This disease-causing process starts in childhood. Children who are exposed to stress early in life are less likely to be healthy throughout their lives. Infants who experienced stressful events and had high levels of the stress hormone cortisol suffered more often from 12 of the 14 most common childhood diseases up until age 10 compared to infants with lower cortisol levels.1
Stress in childhood has effects that can last the rest of a child’s life. Stress reduces the length of telomeres, caps on the ends of your chromosomes. Telomeres stop the chromosomal DNA from unraveling and are often compared to the tips on the ends of shoelaces. Each time a cell divides, telomeres become shorter until eventually the cell is no longer able to divide and dies. One study showed that children who had a stressful childhood had significantly shorter telomeres as adults compared to children who had happier childhoods.2
The Price We Pay for Being Stressed Out
When you’re exposed to chronic stress, your adrenal glands pay the price. The adrenal glands are part of a larger system known as the hypothalamic-pituitary-adrenal axis. This system is made up of three endocrine glands—the hypothalamus, the pituitary gland, and the adrenal glands—which interact to influence the way your body reacts to stress. The hypothalamus and pituitary and adrenal glands are often referred to as the hypothalamic-pituitary-adrenal axis—the HPA axis for short. The hypothalamus secretes vasopressin and corticotrophin-releasing hormone (CRH), which in turn triggers the pituitary to produce adrenocorticotropic hormone (ACTH), which then sends a message to the adrenal glands to produce the stress hormone cortisol.
Balanced cortisol levels are healthy. But chronic stress, like the kind we’re constantly exposed to in modern times, disrupts normal cortisol production, so that quite often cortisol levels are too low or too high. At the beginning stages of stress, the adrenal glands tend to produce an excessive amount of cortisol, so that levels often test very high. On the other hand, over time, the adrenals become “burned out” and produce less and less cortisol. Each of these states can contribute to feeling fatigued and can lead to many different diseases.
When the adrenals are overproducing cortisol this can eventually lead to a number of problems such as an increase in “belly fat.” This excess weight leads to more wear and tear and strain on the body, which in turn causes the adrenals to produce more cortisol to cope with the extra stress, which in turn leads to more inflammation, more weight gain, and more excess stress.
The over-activity of the HPA axis that occurs with aging and the increased production of cortisol are linked to many different diseases, including type 2 diabetes, atherosclerosis (hardening of the arteries), hypertension, dementia, and depression.3 In addition, cortisol levels that stay high for a long time can weaken immunity and contribute to gastric ulcers, headaches, and osteoporosis.4
In response to internal and external stress the body attempts to stabilize itself, a process researchers call allostasis. However, the body pays a price for allostasis, because it has no choice but to try to adapt to potentially harmful situations.5 Prolonged allostasis creates a burden on the body known as the allostatic load. This is one of the ways in which stress damages your body.
Buffers Against Stress
Our adrenal glands serve as a buffer against stress. They accomplish this by producing not just cortisol, but other hormones such as pregnenolone and DHEA. Your adrenal glands are also affected by your hormonal health. Cortisol is made from progesterone, another hormone that’s important for helping the body cope with stress. In both men and women, progesterone drops with age. There is also a drain on progesterone when you are under stress, because the more cortisol your body needs to cope with stress, the more progesterone it needs to produce the cortisol. If progesterone levels are low, then your body may be under fueled, not producing the cortisol you need to handle stress.
This is a problem I often see in my female patients. The modern woman is trying to juggle so many items on her to do list that she’s under a great deal of stress. Consequently, producing all the cortisol she needs to handle stress is depleting her progesterone levels. This drop in progesterone can result in blood sugar issues, anxiety, insomnia—even weakened bones.6 As a woman’s progesterone levels are depleted she won’t have the building block needed to make cortisol and will make less and less of it. And she won’t be able to handle stress.
A drop in progesterone due to the need for cortisol and an imbalance between progesterone and estrogen can affect men, too. The weight gain, low libido, and prostate enlargement that can occur in men during aging are partly due to an imbalance in progesterone and estrogen.
The NeSID Theory
I have proposed a theory called the NeSID (Neuroendocrine Stress Induced Dysfunction), which I am going to discuss in an upcoming issue of the Townsend Letter. This theory describes exactly how stress wreaks havoc on your body and the different mechanisms behind which stress can cause disease. Most importantly, it describes how your body tries to prevent an overly high rise in cortisol levels.
For example, stress increases levels of 5-alpha reductase, the enzyme that transforms the male hormone (androgen) testosterone to dihydrotestosterone (DHT). 5-alpha reductase also helps degrade cortisol to its metabolites. Receptors for androgens are more likely to bind with DHT compared with testosterone. In addition, testosterone detaches from the receptors more readily than does DHT. This can be harmful to health because DHT is associated with male pattern baldness, benign prostatic hyperplasia (BPH), and prostate cancer.7
In obese men and women, insulin resistance causes 5-alpha reductase levels to go up. These elevated 5-alpha reductase levels inactivate cortisol levels in the liver. That’s why researchers have proposed that the rise in 5-alpha reductase is the body’s way of trying to protect against excessively high cortisol levels. However, this approach by the body to defend against high cortisol backfires. It leaves the body at the mercy of the DHT produced.7,8
Not everyone reacts to stress in the same way. For some people, a given situation may elicit anxious feelings while for others the situation is “no big deal.” Some people also can cope with stress better than others. My NeSID theory explains why this is so. Having a greater resiliency to stress has to do with the activity of an enzyme called catechol-O-methyltransferase, encoded by the COMT gene. Catechol-O-methyltransferase helps inactivate the brain neurotransmitters dopamine, epinephrine, and norepinephrine. People can have different variations of the COMT gene and the type of variation a person possesses determines how easily they can cope with and recover from stress.9
How To Protect Yourself from Stress
When I talk to my patients about stress, I usually take a dual approach of recommending stress-reduction strategies while at the same time suggesting nutritional supplements that will help them cope better with stress.
On top of the list of stress-reduction strategies is getting enough sleep. When you are well rested you’re better able to handle stressful situations and sleep loss can cause cortisol imbalances.10 If you snore, have high blood pressure and/or heart disease, or wake up a lot in the middle of the night, having your doctor test you for sleep apnea is a good idea. Sleeping in a dark room also is essential. Additionally, I recommend lessening our connectivity to information overload by turning off email, computers, and cell phones at least an hour or two before bedtime.
There’s also some good evidence in the medical literature that mindfulness mediation and mindfulness-based stress reduction can help relieve insomnia.11,12 Mindfulness meditation is a type of meditation where the person focuses on their breathing and notices in an accepting, non-judgmental way when the mind becomes distracted. Mindfulness-based stress reduction, which combines mindfulness meditation and yoga, was developed at the University of Massachusetts Medical Center.
One of my favorite nutritional supplements to balance cortisol levels and help patients cope with stress is a standardized/patented combination of Magnolia bark extract and Phellodendron bark extract known as Relora®. Studies have shown this combination can lower cortisol and help people feel more relaxed, while encouraging weight loss in people who eat when stressed.13
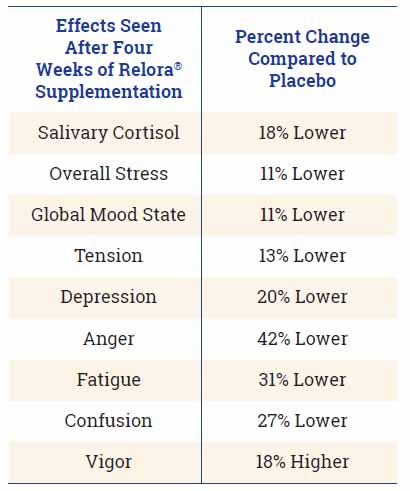
In one study, researchers measured the effects of Relora® on competitive athletes who were under pressure due to their intense exercise routines combined with their daily living activities. After four weeks of taking Relora®, cortisol levels were significantly lower compared to subjects taking the placebo. Subjects taking Relora® were in a better mood and experienced less stress, tension, depression, anger, fatigue, and confusion. They also had more vigor. To see how impressive Relora® was at reducing stress, take a look at the table below, which gives more specifics about the study results.13
Other supplements that I like to use to help lower excessively high cortisol levels include ashwagandha (Withania somnifera) and Rhodiola rosea. In several human studies, ashwagandha has reduced anxiety and stress. For example, in one randomized, double-blind, placebo-controlled study of 64 subjects with a history of chronic stress, ashwagandha root extract significantly reduced stress and serum cortisol levels.14 In a study of Rhodiola, a dose of 200 mg twice daily reduced stress after only three days and even greater improvements occurred after one and four weeks of taking this botanical.15
Another supplement I find to be useful for lowering stress levels is L-theanine, an amino acid found in green tea that can trigger your brain to produce a more relaxed pattern of brain waves. L-theanine can reduce many of the symptoms of stress including a high heart rate.16 I often take L-theanine prior to traveling and other stressful situations and find it has a calming effect.
Take Charge of Your Life
Finally, if we are going to brush off the effects of stress, we should all make every effort to take charge of our lives. We need to actively live our lives, not have our lives live us. We need to refocus on our original goals and dreams, but not allow the pursuit of them to blind us to the fact that each day that we have our health is a day to enjoy and not squander by giving in to the pressures of modern life.
References:
1. Karlén J, et al. Pediatrics. 2015;135:e1450-7.
2. Tyrka AR,et al. Biol Psychiatry. 2009 Oct 13. Published Online Ahead of Print.
3. Martocchia A, et al. Aging Clin Exp Res. 2015 Mar 27. [Epub ahead of print.]
4. Dean W. Neuroendocrine Theory of Aging: Chapter 2. Adaptive Homeostat Dysfunction. www.warddeanmd.com/articles.
5. Picard M, et al. Nature Reviews Endocrinology. 2014;10:303-10.
6. Samaras N, et al. Clin Interv Aging. 2014 Jul 23;9:1175-86.
7. Tomlinson JW, et al. Diabetes. 2008;57:2652-60.
8. Baudrand R, et al. Metabolism. 2011;60:1775-80.
9. Kang JI, et al. Neuropsychobiology. 2013;68:174-80.
10. Leproult R, et al. Sleep. 1997;20:865-70.
11. Black DS, et al. JAMA Intern Med. 2015;175:494-501.
12. Ong JC, et al. Sleep. 2014;37:1553-63.
13. Talbott SM, et al. J Int Soc Sports Nutr. 2013;10:37.
14. Chandrasekhar K, et al. Indian J Psychol Med. 2012;34:255-62.
15. Edwards D, et al. Phytother Res. 2012;26:1220-5.
16. Kimura K, et al. Biol Psychol. 2007;74:39-45.
The content is shared with the understanding that the author and publisher are not engaged in rendering medical, health, psychological, or any other kind of personal professional services. If the reader requires personal medical, health, or other assistance or advice, a competent professional should be consulted.
The author and publisher specifically disclaim all responsibility for any liability, loss, or risk, personal or otherwise, that is incurred as a consequence, directly, or indirectly, of the use and application of any of the contents of this newsletter.


